Researchers develop model of in-hospital mortality for patients undergoing TAVR
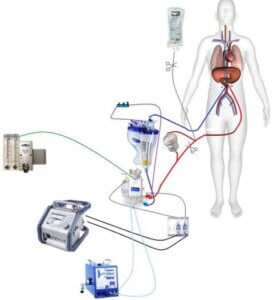
Researchers have developed a model of in-hospital mortality for patients undergoing transcatheter aortic valve replacement (TAVR) using data from the Society of Thoracic Surgeons (STS)/American College of Cardiology (ACC) Transcatheter Valve Therapy (TVT) registry.
The model will be incorporated in the registry’s software and will help select patients who may benefit from TAVR.
Lead researcher Fred H. Edwards, MD, of the University of Florida School of Medicine in Jacksonville, and colleagues published their results online in JAMA Cardiology on March 9.
The researchers noted that TAVR provides a treatment option for patients with critical aortic stenosis who are not candidates for surgical aortic valve replacement, including those at high risk for mortality. They noted that no statistical risk model has been developed for patients undergoing TAVR.
Chesapeake Research Review, Inc., which is the review board for the ACC and STS, approved this study and its protocol and granted a waiver of informed consent. Patients who underwent TAVR all had expected survival of at least one year, according to the researchers.
The TVT registry was launched in 2011 after a national coverage determination from the Centers for Medicaid & Medicare Services required patients undergoing TAVR to participate in a national registry.
“The Steering Committee of the TVT Registry has been committed to the development of a series of risk models that will be based on TVT Registry data,” the researchers wrote. “The initial outcome to be modeled was selected after a thorough review of collected data. In-hospital mortality is a clearly defined outcome with obvious clinical importance and a high degree of completeness, thereby making it the best candidate for modeling at the present time. Subsequent models based on survival of 30 days and longer are planned.”
The researchers developed the model from 13,718 patients who underwent TAVR from Nov. 1, 2011, to Feb. 28, 2014, at 256 centers participating in the TVT registry. Of the patients, 48.9 percent were men, and the mean age was 82.1 years old.
They then validated the model by using a training set–test set approach and assessing records from 6,868 patients who underwent TAVR from March 1 to Oct. 8, 2014, at 314 centers. Of the patients, 51.7 percent were men, and the mean age was 81.6 years old.
The researchers selected candidate covariates by assessing prior literature and gathering expert opinion. Physicians then selected the model risk factors by completing a survey.
The model covariates were age per five-year increments; glomerular filtration rate per five-unit increments; dialysis vs. no dialysis; New York Heart Association (NYHA) class IV heart failure; severe chronic lung disease; nonfemoral access site; and procedural acuity (category 2, 3 or 4).
“The inclusion of nonfemoral access as a covariate bears mention, because nonfemoral access might be considered a departure from the standard practice of including only those factors present at admission,” the researchers wrote. “We considered nonfemoral access to be a marker of increased risk that was nondiscretionary, because the operators were compelled to undertake a riskier approach to access owing to patient factors beyond their control. For this reason, the inclusion of nonfemoral access as a potential covariate was believed to be appropriate.”
Overall, 5.3 percent of patients died in the hospital. The researchers mentioned there was good agreement between predicted and observed in-hospital mortality rates.
They also assessed the model in subgroups based on ejection fraction of less than 35 percent vs. 35 percent or greater; NYHA class IV vs. other than class IV; acuity categories; and a prior aortic procedure vs. no prior aortic procedure.
The researchers noted a few limitations of the model, including that it did not include frailty indices such as the 5-m walk test of gait speed and quality of life measures such as the Kansas City Cardiomyopathy Questionnaire. Although the TVT registry data are subject to internal data quality checks, the researchers mentioned the external audit process was in its early stages.
“This model based on TVT Registry data demonstrates excellent calibration in the overall population and in important clinical subsets,” they wrote. “Model discrimination as measured by the C statistic is higher than that for previously reported models that have been used in the population undergoing TAVR.”
Content retrieved from: http://www.cardiovascularbusiness.com/topics/coronary-intervention-surgery/researchers-develop-model-hospital-mortality-patients-undergoing-tavr.